On Barry Block’s daily PM News (www.podiatrym.com) the other day a colleague presented a case of a neuropathic patient with no wounds presenting with what he felt was osteomyelitis of the 2nd and 3rd metatarsals. Although I did not feel that the case was actually osteomyelitis, a feeling I expressed in a response to that site, I was intrigued by the comment of the original poster that; after giving the patient 8 week of oral ciprofloxacin (another potential misjudgement I discussed in my response), “I just think it is interesting to see how this bone infection responded to very little care.” This comment had me reflecting on what we consider as “Standard of Care” for the treatment of osteomyelitis.
In the 3rd Edition of the Handbook I review the evidence that shows that perhaps we should rethink this “Standard”. The entire concept of 4-6 weeks of IV antibiotics as being some magical bullet that will treat osteomyelitis is based on 30-40 year old animal studies. There is really no human evidence to support that this is the optimum therapy. In fact, much of the recent data that has been presented, particularly out of Europe, suggests that ORAL antibiotics alone with either NO surgery or just “conservative” debridement of infected bone may be just as effective therapy. The literature supporting this approach is actually quite a bit more hefty that that supporting the old traditional “standard”. I explore this question in detail in a lecture I frequently present entitled (thanks to David Armstrong for the catchy title) Antibiotics for Osteomyelitis: Boneheaded or brilliant? One of these presentations can be viewed for free at the website for the always stimulating Diabetic Foot Global Conference (to be held this coming year in Hollywood, CA March 18-20, 2010): http://www.dfcon.com/presentations2009/sat_joseph.html
In no way do I mean to say that surgery is unnecessary. In fact, if ablative surgery can be performed, it is curative without the use of any antibiotic therapy. But, sometimes, patients either do not want, or can’t undergo a surgical procedure. In those cases I am relieved to see that we do have data to support the non surgical treatment of these cases with oral antibiotics alone. Of course, this approach is not perfect and there are still unanswered questions. Probably the greatest is the question of duration of therapy. Do we only need the orals for 4-6 weeks or longer? One study, referenced in the lecture, by John Embil incorporated 41 weeks +/- 31 weeks of therapy! This needs to be addressed. The other literature I would direct you to review is the consensus statement put out by the International Working Group on the Diabetic Foot (IWGDF) http://iwgdf.org whose recent systematic reviews of the diagnosis and treatment of diabetic foot osteomyelitis should be reviewed by everyone treating this condition.
To me, this is one of the most fascinating and important areas that we need to explore in the future.
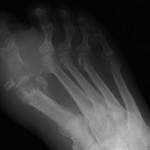
Osteomyelitis of the 1st MTP Joint

