Dr. Todd Divan, a podiatric physician from Potomac, IL, sent me an excellent question via personal email. On the belief that if one person asks a question, many others may be thinking the same thing, I reprint the question and answer here with Dr. Divan’s kind permission.
Dr. Joseph,
I listened to the lecture you have on PRESENT podiatry for the “Diabetic Foot Infections” involving the IDSA classification system. This was excellent. I will also be checking into a slide show share lecture you have placed available online for the “Current Emerging Antibiotics for MRSA”.
I agree that expressing the “tough love” passion with the patient is important. Some of these patients just don’t get it that they are really suffering increased susceptibility to losing a leg or even a life.
I would like to know any journal readings you would highly recommend regarding this topic. I have a few thoughts to share. For example, do we as podiatrist need to worry about Proteus, Serratia, Klebsiella, E. coli, or Citrobacter in the diabetic foot infections? You mentioned a study which gave the impression we don’t have to worry too much about treating Pseudomonas aeruginosa because there is a fairly high cure rate with the Pseudomonas when treated with a 1st gen cephalosporin (an interesting thought). However, I think the point should be emphasized to avoid applying this concept across the board on Gram neg infections, with the thinking that they will heal secondarily alongside of therapy focused on Gram pos infections. My thinking is based a great deal on the fact that once we have taken a culture and the presence of a certain bug is documented in the chart, if we don’t treat because of this concept, then an infection turn bad (and sometimes fast). I am worried this type of complication could lead us into a higher risk case and expose the practitioner to increased legal liabilities. Shouldn’t I have to follow the tendency of the infectionist in my area, since working on a multidisciplinary basis is important. I did pick up on your point that using aztreonam or the like (depending on the culture report) could provide good combination therapy to get coverage for the Gram neg infections.
Thank you for your contributions. Much appreciated.
Todd Divan, DPM
MY RESPONSE
Todd,
Thank you for the kind words and the thoughtful questions. I have attached a copy of the Infectious Diseases Society of American Diabetic Foot Guidelines where we go into the concept of gram positive organisms in more detail. This paper was published in 2004 and we have a new manuscript in the works, hopefully for publication summer of 2010. The primary importance of gram positive infections does not change with the new document.
When you read the guidelines you will see that we stress the primacy of aerobic gram positive cocci as the major causative organism. This is particularly true in mild and many moderate infections. We do say that as the infection becomes more severe, if there is the presence of necrotic tissue, or of the patient has been exposed to previous courses of antibiotics, then gram negative aerobes and anaerobic organisms become more prevalent. Even if you culture these organisms, the evidence is not clear that you have to treat them. Tony Berendt, Ben Lipsky and I refer to this as the “head of the snake” philosophy. In other words, Staph and Strep make up the “head of the snake” and the other bugs you list below make up the body. If you “cut off the head” i.e. use antibiotic therapy directed at the Staph and Strep, then the “body” dies. Again, this is primarily true of the mild and moderate levels. We are NOT advocating only using gram positive coverage for the more severe infections.
Even with this concept, and it is just that, a concept, even though it is based in excellent data, I tend to start empirically with broad spectrum coverage (perhaps partly for the legal exposure reason you mention below). In the case with our hospital I even need to use MRSA coverage. Almost all patients are begun on Zosyn + Vanco. Certainly Invanz can be substituted for the Zosyn and Zyvox for the Vanco depending on your local formulary. Please note I do NOT use the Zosyn for Pseudomonal coverage. I am still of the FIRM believe that no evidence supports needing to cover Pseudo empirically in just about any diabetic foot infection. In fact, I don’t remember the last time I even grew that bug from a DFI.
Regards
Warren
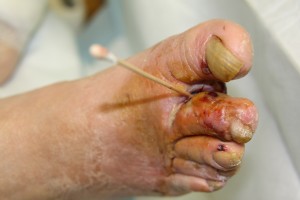
IDSA Moderate DFI

