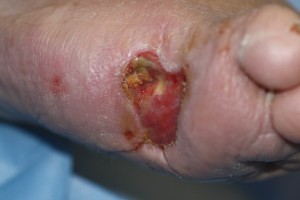
Bone exposed through an open ulceration
If I were to ask any reader of this blog the proper technique for harvesting a bone culture I am fairly certain that the common response would be that it must be a) not taken through the ulcer or sinus tract b) taken from a separate clean site c) the patient should be off all antibiotics. In fact, ever since Mackowiak published his seminal paper in JAMA way back in 1978 showing sinus tract cultures had poor concordance with deep bone cultures; the prevailing wisdom has been that sinus tracts (and thus ulcers) were off limits. These results were further confirmed by Eric Senneville in 2006 and Khatri in 2001 along with others. Thanks to these studies, it has become common knowledge that a proper bone culture should never be harvested through a sinus.
The question of whether or not the patient needed to be off of all antibiotic therapy prior to the culture was always less clearly delineated. It was almost an empirical belief that if a patient was on antibiotics at the time of the culture then the results would be unreliable. After all, if a culture is reported as showing “no growth” was this because the specimen was poor, the patient never had osteomyelitis in the first place, or the antibiotics had prevented the organism from growing?
A recent study by Louis Bernard and colleagues out of University Hospital of Geneva Switzerland, and published in the September 6, 2009 issue of the International Journal of Infectious Diseases challenges much of what we currently hold as sacrosanct. In this non-randomized, prospective trial 141 patient with 154 episodes of osteomyelitis each underwent 4 microbiological samplings. Sample “A” consisted of 2 consecutive sinus tract cultures with bone contact (“A1” & “A2”) after only local cleansing of the sinus tract with 0.9% saline. Sample “B” consisted of a surgical bone biopsy through the sinus. Sample “C” was a surgical biopsy obtained through an uninfected sited, referred to as the “gold standard”. Their results showed that when both sinus tract cultures “A1 & A2” revealed the same organism the concordance between “A” and gold standard “C” was 96%. They calculated the sensitivity as 91%, specificity as 86% and accuracy as 90%. On top of that, they found that the result was not affected depending on whether the patient was on antibiotics prior to the cultures or not.
In their Discussion the authors go out of their way to state that “in no way should these consecutive deep sinus tract specimens replace bone culture in situations where a biopsy can be readily obtained because bone culture remains the gold standard for the microbiological diagnosis of osteomyelitis”. There are sometimes, however, when a surgical culture is just not practical and that patient has already been started on antibiotic therapy, as the authors call it “clinical reality”.
This fascinating work challenges our common thinking about how to harvest microbiological specimens for osteomyelitis diagnosis and treatment. I urge the readers of this blog to search out this paper and read it. It is new, innovative, evidenced based works such as this that lead me to wanting to create a blog…so that I could keep those interested readers up to date on current thinking between editions of the book.

